My Bichon Sparky was an amazing dog. We originally adopted him from a breed-specific rescue after he’d endured months of neglect — including being chained continuously to a backyard grill. In the end, he lived to be a treasured member of our family for nearly 21 years. Together we experienced a range of miraculous joys and unexpected challenges. One of the most unnerving of these challenges was pancreatitis.
Essentially, canine pancreatitis occurs when a dog’s pancreas becomes inflamed. The pancreas, which is situated on the right side of the abdomen just next to the stomach, is a vital organ, which produces enzymes that help with food digestion. It also secretes hormones such as insulin, which regulates blood sugar. When pancreatitis strikes, these digestive enzymes are often released prematurely and can begin to corrode the actual organ itself.
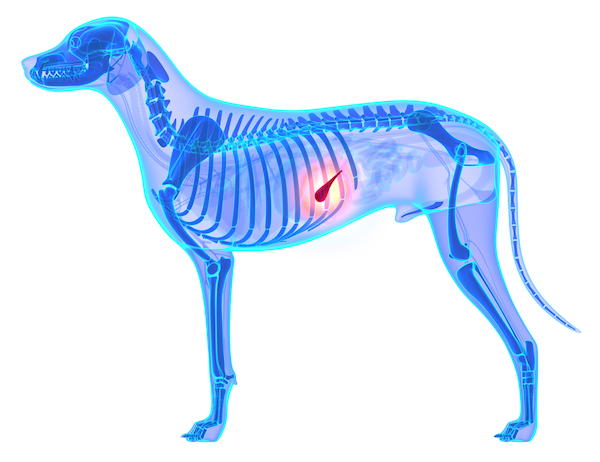
According to my vet, the enzymes can also spill over into the abdominal cavity, which may cause secondary damage to the liver, bile ducts, gall bladder, and/or intestines. A dog who recovers from one bout of pancreatitis can sometimes experience recurring episodes. If secondary organ impairment occurs, then digestion may be compromised for the rest of that pup’s life.
Because of Sparky’s affectionate yet relatively low-key personality, we weren’t initially concerned one winter when he began acting a little sluggish. At first he simply seemed bored of playing fetch; but then one day, he also refused to finish his food. I’ve found this to be one of the most exasperating problems with canine pancreatitis: While initial onset is sometimes severe, it can often be surprisingly subtle. Unfortunately, those unobtrusive early symptoms can hint at a great deal of internal damage silently taking place.
Soon our Sparky took an alarmingly abrupt turn for the worse. He began to experience abdominal tenderness, diarrhea, and violent nausea, which caused our dog to vomit a thick yellowish liquid repeatedly, despite having no food in his stomach. This prompted a frantic midnight trip to the emergency vet, where Sparky was placed on immediate IV antibiotics, anti-inflammatories, and fluids in an urgent effort to save him.

I learned that when the pancreas becomes overly inflamed, it’s usually necessary to rest it by withholding all food and liquid taken through the mouth. In acute-onset cases, dogs can often go into systemic shock and require high doses of IV fluids and medications in an attempt to revive them. Sparky was hospitalized for nearly five days while a host of IV preparations were administered. Oral nourishment was reintroduced at a snail’s pace — first liquid, then puree, and finally tiny chopped morsels every few hours by hand.
We were, of course, incredibly lucky with Sparky, and he survived for many years. However, his battle back to wellness compromised his digestion for the rest of his life. I’d like to share the key lessons we learned from pancreatitis, so other pet parents can take action if they notice unusual behavior:
- Early signs of this ailment may include any combination of general tiredness, weakness, dehydration, abdominal tenderness, fever, weight loss, vomiting and/or diarrhea. If you notice anything atypical, monitor your pet very carefully.

- According to our vet, there’s no truly significant age, gender, or breed-specific disposition to pancreatitis. In other words, any dog could potentially be at risk.
- Our vet mentioned that certain drugs may increase a dog’s susceptibility to pancreatitis. This does not mean a dog will automatically contract the ailment if these drugs are administered; it simply means that pet parents should be on guard. These medications can include anti-seizure drugs such as potassium bromide or phenobarbital, catabolic steroids such as prednisone, and diuretics such as Lasix (furosemide).
- Pancreatic inflammation can be diagnosed through a blood test called the PLI (pancreatic lipase immunoreactivity) test. This measures two pancreatic enzymes, lipase and amylase, that can sometimes become elevated when animals have pancreatitis. The vet tech told us that slight inflammation does not necessarily mean pancreatitis. However, when such inflammation is detected along with symptoms mentioned above, an ultrasound may be called for and rapid medical intervention may be necessary.

- Pancreatitis can definitely recur. In fact, Sparky sustained so much digestive damage from his initial bout that he struggled with lifelong pancreatic inflammation and enzyme imbalance.
We also found a holistic vet who shared some eye-opening guidelines. In my opinion, these insights were critical to preserving Sparky’s quality of life and gradually returning him to wellness. She suggested that we:
- Minimize fats and limit treats, which can reduce overall pancreatic load.
- Provide plenty of fresh water, even a pet fountain that encourages regular hydration.

- Reduce dietary carbohydrates. These prompt the release of insulin and can be extremely taxing to the pancreas as it tries to balance blood sugar levels. We began feeding Sparky low-fat, species-appropriate recipes by Dr. Richard Pitcairn, which we simply made at home and froze for convenience. Sparky also loved Merrick and Tiki Dog canned foods, all-natural formulations made with human-grade meats.
- Reduce or eliminate highly processed foods for the same reason. Many dried commercial kibbles, for instance, are processed at extreme temperatures that destroy vital nutrients and enzymes. A diet too heavy in these foods can hold the pancreas in a chronic state of low-grade inflammation, at which point it’s more susceptible to pancreatitis.
- Provide an added source of daily digestive enzymes. In our case, we sprinkled Wholistic Pet Digest-All Plus powder on Sparky’s food. Even though we’d reduced general carbohydrates, these enzymes gave his pancreas an extra boost to help process his food.
- Encourage daily activity at a comfortable level. This helps boost metabolism, eliminate waste, and keep cortisol levels controlled.
Pancreatitis can be a life-threatening condition and, as we learned the hard way, its onset can be remarkably subtle. But Sparky’s long life is proof that by staying informed, aware, and observant, we pet parents can help to protect our furry friends and decrease the chances of serious damage occurring. It definitely pays to pay attention.
Read related stories on Dogster:
- What Does Pancreatitis Do to Dogs?
- Ask a Vet: Is It Safe for Dogs to Share Thanksgiving Feasts?
- Can Dogs Eating Chocolate Cause Long-Term Health Problem?
About the author: Marybeth Bittel is a freelance writer who lives in the Midwest with her wonderful husband, her crazy rescue dog Grant, and her level-headed rescue dog Maizy – all of them Heinz 57 mixed breed types. Marybeth identifies as mostly Italian, so she enjoys feeding family, friends and furkids almost as much as Grant and Maizy enjoy eating. She’s also a marketing communications consultant and former marketing/PR exec. Connect with her on LinkedIn or — to see her latest pet pics (and be careful what you wish for here) — check out her family Instagram feed.
Featured Image Credit: damedeeso | Getty Images.









