Thrombocytopenia is the scientific term for a low platelet count. Platelets make up the normal components of the body’s blood, and they help to form blood clots. Platelets are one of the first lines of defense to prevent bleeding. Thrombocytopenia refers to a decreased platelet count, therefore putting your dog at risk for bleeding. Immune-mediated thrombocytopenia (IMTP) happens when the body’s immune system attacks its own platelets. In this article, we’ll discuss what immune-mediated thrombocytopenia is, what are the signs your dog may have it, and how it’s diagnosed and treated. Thrombocytopenia can affect any dog of any breed and size, and it’s important to know about this disease.

What Is Immune-Mediated Thrombocytopenia?
Platelets are a type of blood cell produced in the bone marrow that circulates in the bloodstream. Platelets are one of the first types of blood cells that arrive to help form a blood clot and stop bleeding. This can be bleeding that is external, such as a cut in the skin, or internal such as a stomach ulcer.
Platelet numbers can be decreased due to a number of reasons including decreased production or simply consumption (they are all used up in times of excessive bleeding). But for the purposes of this article, we’re going to talk about decreased platelet numbers due to immune-mediated destruction.
The immune system functions to recognize threats to the body such as bacteria, viruses, and different types of fungus. Through a complex system of checks, balances, and triggers, the immune system is activated to attack and remove these different threats. This helps to keep the body safe from infection. However, sometimes the triggers and/or checks and balances in a dog’s body are off, causing the body to view its normal cells as foreign. This is what happens in immune-mediated thrombocytopenia (IMTP). The dog’s normal immune system, for whatever reason, starts to view platelets as foreign threats to the body, and it will start to destroy the platelets.
We can see immune-mediated disease with other cells such as red blood cells and white blood cells. IMTP is especially dangerous in dogs as it puts them at risk for life-threatening hemorrhage.
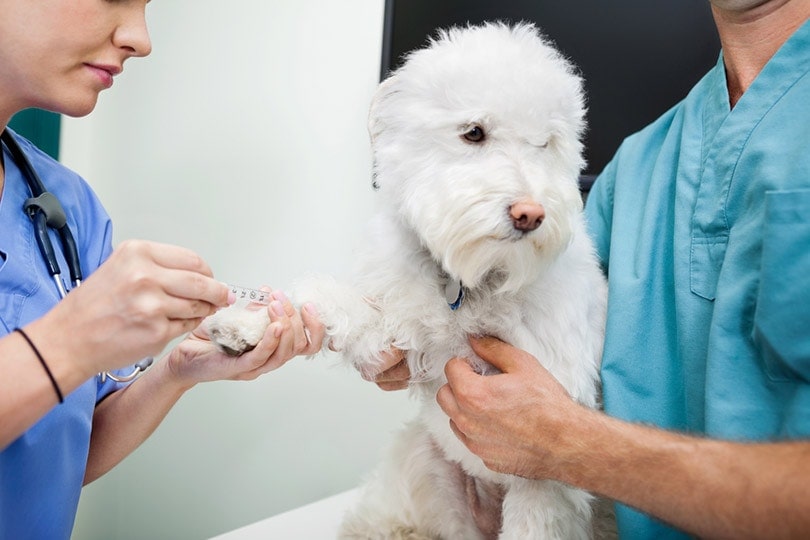
What Are the Signs of IMTP?
IMTP signs may or may not be obvious to you. However, your veterinarian may notice subtle changes on their physical exam that will cause them to be concerned. The most common signs of IMTP are pale gums and/or mucous membranes with areas of bruising. These small, splotchy red areas are known as petechiation and can typically be seen within the mouth, ear pinna, or even over the belly and groin. Larger areas of bruising are called ecchymoses and can be seen in similar areas.
Some dogs will start to have bleeding from unusual places and/or bleeding not associated with any type of trauma. In other words, some dogs will bleed from the mouth, have blood in their urine, and blood from their eyes and/or nose. Your veterinarian may notice that a simple blood draw bleeds excessively and/or forms a large area of bruising. Other times, bleeding may be internal and not be visible to the naked eye. Your dog may develop bleeding within their chest, causing them to have difficulty breathing. Bleeding can also occur into the GI tract, causing either bloody vomit, or black, tarry stools when your dog defecates.
Your veterinarian can determine if all of these signs are related to IMTP by completing bloodwork to know an exact platelet count on your dog.
If you are far from a vet clinic and need urgent vet advice and guidance on the best course of action you can chat with a vet online.
What Are the Causes of Immune-Mediated Thrombocytopenia in Dogs?
One of the more frustrating things about these cases for veterinarians is that we often do not find a cause. This is known as a diagnosis of exclusion. In other words, your veterinarian will need to rule out any of the other causes of IMTP before coming to a conclusion about what triggered it. Still, no trigger may be found – this is known as idiopathic.
IMTP can also occur secondary to another underlying disease. This is known as secondary IMTP and can occur from cancer, tick-borne disease (such as lyme disease), certain drugs, severe bacterial and fungal infections, and even multi-organ shut down. Contrary to popular belief, IMTP has not been consistently shown to be associated with vaccines. Our canine vaccines have been well studied and improved over the years that we do not commonly see secondary IMTP from administration.
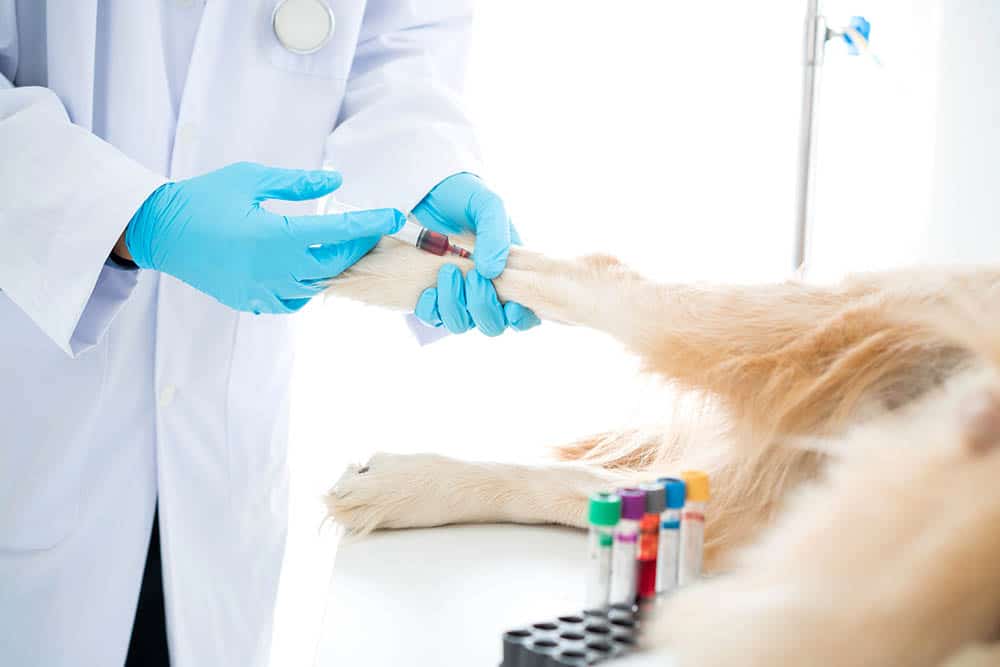
How Do I Care for a Dog With IMTP?
The first thing you will need to do is get an accurate diagnosis from your veterinarian. This will include bloodwork and likely a manual platelet count. In other words, the blood will be examined on a microscope slide to manually count the platelets, not just rely on what a machine says. After the bloodwork results, your veterinarian may also recommend further tick testing, radiographs, and ultrasound to rule in/out all of the other causes of IMTP we discussed above such as tick-borne disease and cancer.
If there is an underlying disease present – fungal infection, bacterial infection, cancer or tick-disease – then your dog will need to be treated for that disease in order for the platelet count to improve. Your dog will also need to be put on aggressive medications to reduce the immune-response. This is achieved by high doses of steroids in combination with immune-suppressive medications such as Cyclosporine or Azathioprine. These drugs help to decrease the aggressive attack on platelets by the body’s own immune system.
While on these medications, your dog will be susceptible to infections and injuries as their immune system is not able to fight off any attacks. Your dog will need to be closely monitored by your veterinarian for both infections and any changes to their platelet count with regular bloodwork. Your dog will be on medications for months before they can be weaned down. Some dogs will eventually be able to be completely weaned off medications, while others are on medications life-long.
Your dog will need to be kept extremely quiet while their platelet numbers are low. Once the platelets drop below a critical point, any animal is at risk for spontaneous hemorrhage and death. If your dog has no platelets and they start to bleed, they have no defense to stop that bleeding. No matter what medical intervention is done, if your dog physically does not have the cells in their body to form a blood clot, they will die.

Frequently Asked Questions
Can My Dog Be Cured?
Yes and no. This depends on if the cause is primary (often idiopathic) or secondary. Your dog has a much better chance of being cured if they have secondary IMTP and the underlying disease can be cured such as a bacterial or fungal infection. With idiopathic, we never know how and when the body will respond, and if your dog will go into remission or not. There is a risk of life-long IMTP and many affected dogs will pass away.
Can’t My Veterinarian Just Inject More Platelets into My Dog?
No. This is not a thing in veterinary medicine. If your dog has IMTP that causes them to bleed, therefore dropping their red blood cell count, then a blood transfusion can be completed. This will help to improve circulation, oxygen delivery, and overall health. However, there is no way to collect and administer just platelets to your dog if they are decreased.

Are There Side Effects to the Medications?
Yes, the medications are not without significant side effects. As discussed above, your dog will be prone to secondary infections due to a decreased immune response. High doses of chronic steroids are notorious for causing muscle wasting, increased drinking/urinations, hair loss, and pot-bellies. Other immunosuppressive drugs may cause nausea, vomiting, diarrhea, and generally decreased appetite. Unfortunately without these medications, your dog’s immune system will continue to attack their own platelets.

Conclusion
Thrombocytopenia refers to a decreased number of platelets in the body. The platelets help to clot blood and prevent life threatening episodes of bleeding. With immune-mediated thrombocytopenia (IMTP), the platelets are decreased because the body’s own immune system views them as foreign. The immune system will then attack and destroy them. This will put your dog at risk for bruising, bleeding, and even death.
Your veterinarian will need to diagnose this disease through blood testing, and then run additional diagnostics to determine if there is an inciting cause or if it’s idiopathic. Once diagnosed, your dog will need to be on aggressive immune-suppressive medications for months, potentially lifelong. Unfortunately, this disease is not without risks, and many dogs will not improve or end up passing away. Even if successfully treated, your dog may be at risk for coming out of remission.
Featured Image Credit: hedgehog94, Shutterstock