In this article
Dogs of any age and breed are at risk for the development of autoimmune disease. Not every autoimmune disease is created equally, and not every autoimmune disease has significant life-threatening implications. Unfortunately, some autoimmune diseases can severely impact our canine companions. If this topic sparks your interest or is of concern to you, continue reading to learn more about autoimmune diseases in dogs.

What Is an Autoimmune Disease?
In normal situations, inflammatory cells target and attack external threats like bacteria, viruses, abnormal cells, etc. However, with autoimmune diseases, the body recognizes its own cells and proteins as a threat and generates attacks.

What Causes an Autoimmune Disease?
Currently, it is assumed that there are genetic and environmental/external triggers that influence autoimmune disease in individuals. The factors that may result in disease depend on the autoimmune at hand. For instance, ultraviolet light and some medications have been associated with the onset of skin autoimmune diseases.
Immune-mediated hemolytic anemia is a serious condition in which the body starts destroying its own red blood cells, leading to anemia. This can occur without being provoked, but it can also occur secondary to vaccination, certain parasites, toxins, and other things.
What Are the Signs of an Autoimmune Disease?
The signs of disease vary greatly. Depending on what organ system is impacted by the disorder, signs can be different. For example, animals dealing with immune-mediated hemolytic anemia may experience lethargy and weakness secondary to the anemia. Animals suffering from pemphigus foliaceus may experience dry, discolored skin around the nose. For another example, dogs with KCS or keratoconjunctivitis sicca, also called dry eye, may not have any other signs except for decreased tear production.
Additionally, autoimmune disease can occur sporadically, meaning clinical signs are not always present.
- Fever
- Lethargy
- Change in appetite
- Weakness
- Chronically inflamed skin
- Pain
- Vomiting/diarrhea

Examples of Autoimmune Diseases
- Masticatory myositis
- Dry eye
- Glomerulonephritis
- Myasthenia gravis
- Immune-mediated thrombocytopenia
- Immune-mediated hemolytic anemia
- Lupus
- Pannus
- Pemphigus
If you are concerned about the health and well-being of your pet, seek veterinary advice for the best course of action.
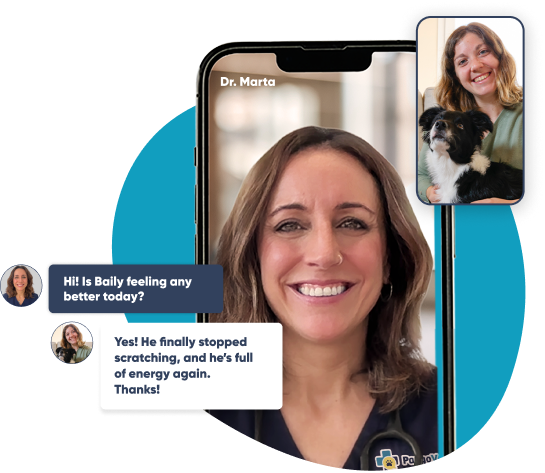
If you need to speak with a vet but can't get to one, head over to PangoVet. It's our online service where you can talk to a vet online and get the advice you need for your pet — all at an affordable price!
Breed Predispositions
Breed predispositions do exist for certain autoimmune disorders. For instance, pannus, an ocular disease, is notorious for occurring in German Shepherds. Lupus may be more likely to occur in Old English sheepdogs and Shelties. Meanwhile, breed predisposition to IMHA exists in Old English Sheepdogs, Poodles, Irish Setters and Cocker Spaniels.

Diagnosing Autoimmune Disease
Just as the signs of an autoimmune disease vary, so do the diagnostic tests used to determine the disorder.
Diagnostics used are dependent on the organs impacted. For instance, pemphigus or lupus, which are two disorders impacting the skin, will require a skin biopsy for a definitive diagnosis. KCS, or dry eye, is an ocular disease that can be diagnosed through testing tear production.
Treatment
Immunosuppressant Therapy
Due to the variety of disease processes autoimmune disorders cause, treatment also varies. However, many disease processes focus on a common trend: reducing the inflammatory response. This has historically been accomplished with steroids dosed at immune-suppressive doses. Unfortunately, steroids often have undesirable side effects, like an increase in appetite and urination. Other medications, like tacrolimus, cyclosporine, and azathioprine, can offer similar immune suppressive results.
If steroid side effects are too unfavorable, another immunosuppressant drug may be added to your companion’s regimen, and the steroid dose may be reduced. Similarly, if the response to a monotherapy is not good, additional immunosuppressants will be added on.
When immune-suppressive medications are used, they cannot be discontinued abruptly. This is because the body may negatively respond to the withdrawal of the medication. Furthermore, if immunosuppression is lifted too quickly, a relapse in disease may occur. Although relapses are possible, tapering and possible discontinuation of medication is the goal. In some autoimmune disorders, lifelong medication may be needed.

Additional Care
Depending on the diagnosed condition, additional therapies may be needed. For example, IMHA may require hospitalization and blood transfusions. Autoimmune diseases may often require antibiotics due to secondary infections.
Monitoring
Due to the nature of autoimmune diseases, frequent monitoring by your veterinarian will be necessary. Immunosuppressant drug therapies needed to overcome disorders may predispose to other infections like urinary tract infections. Laboratory tests will need to be completed routinely to check for secondary infections and response to treatments.

Frequently Asked Questions (FAQ)
My Pet Has Recently Been Diagnosed With an Autoimmune Disease. Will They Require Immunosuppressive Medications Throughout Their Life?
Not necessarily! Some disorders may only require medical intervention during flare-ups or temporarily. Typically, animals battling autoimmune disorders will require a slow taper of immunosuppressive medications before being discontinued completely.

My Pet Has Been Diagnosed With an Autoimmune Disease. Should I Avoid Future Vaccinations?
Some autoimmune diseases may be stimulated by vaccinations, but that is not the case across the board. Determining if vaccinations are recommended for your pet will require a conversation with your veterinarian.

In Conclusion
Autoimmune disease can occur in any breed, although some breeds are predisposed to certain disorders. Diagnosing autoimmune diseases can require several diagnostic tests, and treatments can vary. Additionally, the overall prognosis is dependent on the diagnosed disease. Dogs placed on medication will need to be monitored closely prior to medication adjustments, and owners will need to work closely with veterinarians to manage the patient’s care.
You might also want to know about:
Featured Image Credit: Taps Das, Shutterstock




















2 Responses
Thank you for the information on auto immune diseases. I am reading articles and trying to gain more information to be more effective in seeking treatment of my 3 yr old husky mix. I want to know how to be more successful in treatments so that she will enjoy a better quality of life. She has been seen by a vet for 3 Mo. now and I'm concerned she isn't showing any improvement with her sensitive skin pain. I want to give her a better life than the pain she is currently experiencing.
Thank you for reaching out to us, Everett. I’m so sorry to hear about the challenges your husky mix is facing. It's clear that you're deeply committed to helping her live a better quality of life, and that’s truly admirable. Autoimmune diseases can be incredibly complex, and I completely understand how frustrating it must be to see your dog in pain without significant improvement despite treatment.
I recommend booking a consultation with one of our vets at PangoVet. This way, you'll be able to share all the details of your dog's condition, and they can assess the situation more thoroughly and address any questions or concerns you may have. You can easily book an appointment at a time that works for you using this link: https://pangovet.com/schedule-appointment/.
I hope this helps, and I wish you and your dog the best in finding a path to healing. 🙂