It’s a unique and harsh sound; a honking cough that makes you think a flock of geese is flying overhead. Unfortunately, it’s coming from your little dog, increasing in intensity when they get excited. A honking cough is a classic sign of a collapsed trachea, something that is a fairly common occurrence in our favorite fluffy companions. While the noise alone may make you want to seek treatment, it’s important to know that if a collapsed trachea becomes severe, it can lead to a respiratory emergency.
So, what is a pet parent to do? Read on to find out.

What Is a Collapsed Trachea in Dogs?
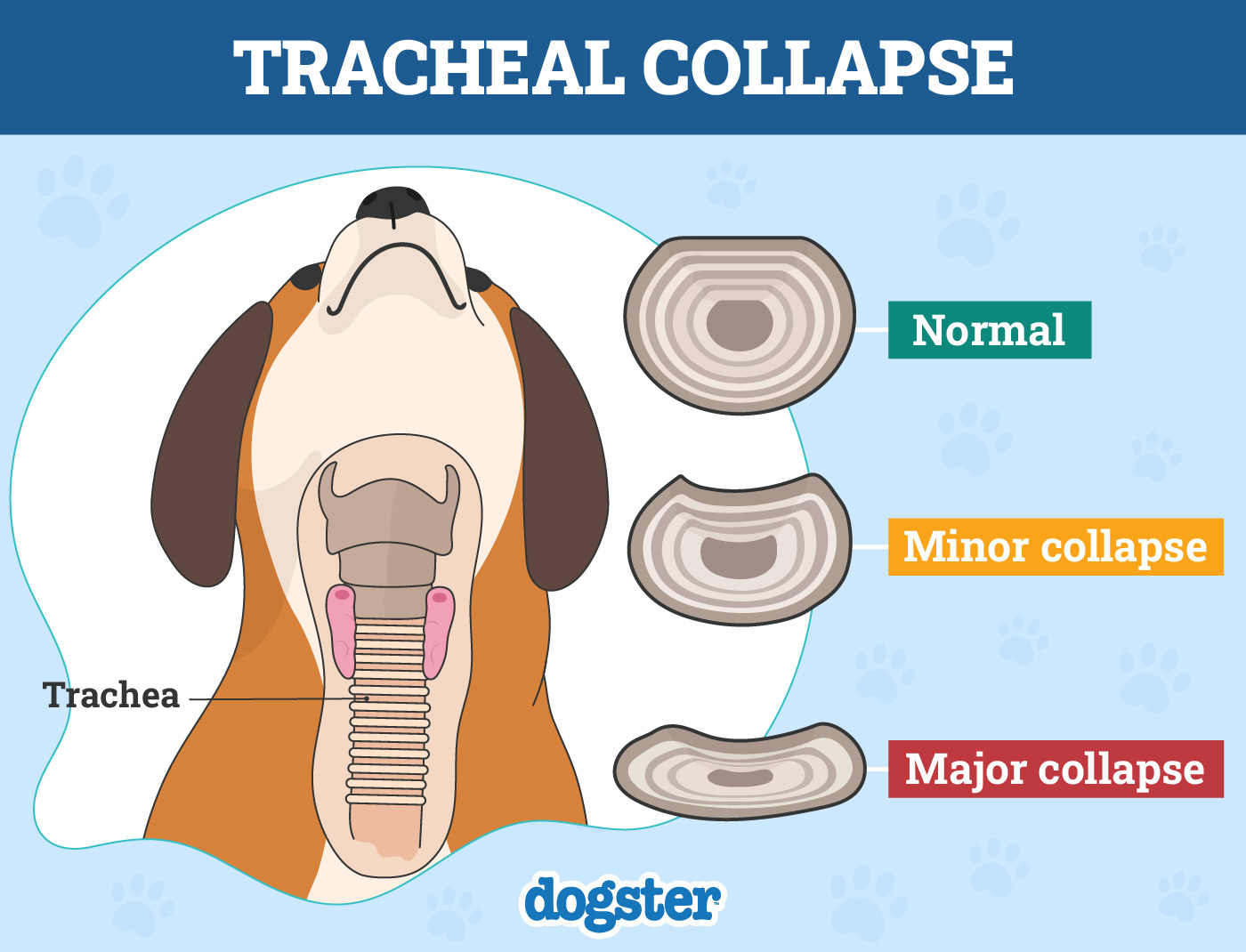
We’ll start with a little anatomy lesson upfront. The trachea is the windpipe that carries air from the throat to the lungs. It’s made up of incomplete cartilaginous rings stacked on each other. The cartilage forms a firm C-shape with a thin tissue membrane completing the ring. This cartilage is designed to hold the trachea open so that air can pass freely.
Dogs with tracheal collapse have weakened cartilage or a saggy membrane. When the cartilage is weak, its rigidity is compromised, causing the trachea to flatten. When the membrane is saggy, it can droop down into the windpipe. Either way, what you’re left with is an airway that was once wide open and is now narrowed or even closed off in some areas when a dog tries to breathe in.
A collapsed trachea can make it difficult to breathe, reducing the amount of air that a pup can draw in with each breath. The change in the shape of the trachea can also create a dry, honking cough, especially when a dog gets excited or stressed and their respiratory rate increases.
Any dog can develop a collapsed trachea, but it is more commonly seen in small breeds, such as Pomeranians, Yorkies, Chihuahuas, Toy Poodles, and Shih Tzus. It is also often a middle-aged to old dog issue, seen more commonly between 4-14 years, but any age is fair game.
What Are the Signs of a Collapsed Trachea in Dogs?
The first thing you’ll most likely notice is that goose-honking cough. It will be dry, sort of like they’re trying to cough up something in their throat. The cough will likely be more common when your pup’s respiratory rate increases, such as with exercise, stress, heat, or excitement, or when pressure is put on the throat from your hand or a collar.
Often, the coughing will stop once your pup catches their breath and has a chance to calm down.
- Difficulty breathing
- Wheezing
- Blue gums or tongue
- Fainting
If your dog’s collapsed trachea is severe enough to elicit the above signs, see your veterinarian immediately.
Your dog’s signs will often coincide with the grade of tracheal collapse that they have. These grade numbers I–IV coincide with the degree to which the trachea is compressed. Grade I is the mildest, while grade IV is the most severe. These grades may be used by veterinarians to best determine your dog’s treatment.
If you are concerned about the health and well-being of your pet, seek veterinary advice for the best course of action.
If you need to speak with a vet but can't get to one, head over to PangoVet. It's our online service where you can talk to a vet online and get the advice you need for your dog — all at an affordable price!

What Are the Causes of Collapsed Trachea in Dogs?
Tracheal collapse is one of those issues that we wish we had a better answer for. More often than not, we won’t entirely know the cause, just that there may be a genetic component since certain breeds develop it at a higher rate than others.
Since it develops most commonly in middle-aged to older dogs, there also seems to be a progressive component. In some cases, a crushing injury to the trachea can lead to collapse, and the signs seen with it, or a dog may be born with a deformed trachea that leads to similar signs.
No matter the cause, other conditions, such as obesity, heart disease, respiratory disease, respiratory irritants, and heat and humidity, can make signs worse.

How Do I Care for a Dog With a Collapsed Trachea?
Treating a collapsed trachea is often aimed at managing it rather than fixing it. It’s going to take some adjustments and potentially medication for the life of your pup.
- Cough medications
- Anti-inflammatories
- Corticosteroids
- Anti-anxiety medications
- Bronchodilators
- Sedatives
You may also want to make some lifestyle adjustments, such as using a harness instead of a collar, achieving and maintaining a healthy weight, and reducing exposure to respiratory irritants like smoke.
You may also find it helpful to decrease your pup’s stress and anxiety with a regular schedule, giving them a safe place to retreat when nervous, and regular exercise and one-on-one interactions. You can try to curb your dog’s bounciness and excitement by putting them in a crate or other room when visitors arrive, or the mail person stops by. You may also want to crate them while you’re away so that your arrival home isn’t met with a loud honking cough.
In some cases, surgery may be attempted to place different types of rigid implants in the trachea to help keep it open. Dogs will often still need some amount of medical management, even with surgery. These surgeries are typically only undertaken by specialty clinics or veterinary teaching hospitals.
Dogs with tracheal collapse, especially in severe cases, are at risk for distressing respiratory episodes, so it’s important to keep regular veterinary appointments for your vet to assess your dog’s condition and adjust treatments as necessary.

Frequently Asked Questions (FAQ)
Is a dog with a collapsing trachea in pain?
Mild cases of collapsing trachea usually aren’t painful; however, the persistent coughing in more severe cases can create inflammation in the airways, potentially causing a sore throat.

How long can a dog live with a collapsed trachea?
Most dogs with tracheal collapse can live a normal life with proper treatment. However, it will require some lifelong adjustments and potential medication for this to happen. You’ll need to work closely and regularly with your veterinarian to ensure that you are doing the most you can to manage this issue.
Can tracheal collapse cause death in dogs?
When a dog is having breathing difficulty related to tracheal collapse, calming them down or administering medications will usually help them breathe better. However, if a dog is severely affected and measures aren’t taken to relieve some of the difficulty, it can lead to severe respiratory distress and death.

Conclusion
A collapsed trachea is, unfortunately, a fairly common issue among our little canine companions. When your dog has a collapsed trachea-related coughing episode, it can be very alarming and even dangerous for your pup. If you suspect that your dog has a collapsed trachea, talk to your vet right away. They will be able to formulate a treatment plan and lifestyle changes that will be necessary to help your dog breathe easily for years to come.
Featured Image Credit: Sanyalux Srisurin, Shutterstock